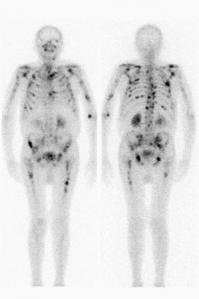
Bone Scan
What is a bone scan?
A bone scan, or bone scintigraphy, is an imaging test. It is used to see problems or damage in your bones. It looks at your whole skeletal system, checking for disease or infection.
A bone scan is often done so that your provider can have "functional imaging" of the bones. Functional imaging measures the rate of bone metabolism. Bone metabolism is the process of how your bones break down and rebuild themselves. If your bone metabolism is high, it can be because of infections, fractures (breaks), or some cancers.
Bones scans are a type of nuclear medicine scan, meaning it uses a radioactive substance. A safe amount of radioactive substance is put into a vein. The radioactive substance goes to areas of bone damage and shows spots where your bone cells are trying to fix the damage. If you have an infection, fracture, or cancer, your body naturally tries to fix it. Your bone cells (called osteoblasts) make more bone and this new bone activity (metabolism) is what is seen on the bone scan. A bone scan may be used when cancer is first diagnosed to see if the cancer has spread to the bone (metastasized).
It is important to know that without talking to you and knowing your medical history, the results of a bone scan can be very hard to understand. For example, old bone injuries can show up on the scan as an abnormal finding.
How do I prepare for a bone scan?
There is usually nothing for you to do before a bone scan. If you take a medication that contains bismuth, like some medications used for an upset stomach or ulcers (ex.- Kaopectate, Pepto Bismol, Maalox, etc.), ask your provider if you need to stop taking the medication before the test.
How is a bone scan done?
An intravenous line (IV, into a vein) is placed, and the radioactive substance (usually Technitium-99m-MDP) is given. This is called the tracer.
- If the scan is being done to look for a bone infection, images will be taken right after the radioactive substance is given, and again 3-4 hours later.
- If the test is being used to check for bone metastases (cancer that has spread to the bone), images are taken only once, 3-4 hours after the injection.
After the tracer goes through your body, you will be asked to lie on a flat table. A camera will move slowly around your body to take pictures. You may be asked to change your position. The scan will check your whole body at once, and this can take up to an hour. A computer processes the images taken to create a picture of your whole body. Any areas with higher bone activity (metabolism) show up as a dark spot on the image (see example below).
Are there any side effects?
There are often no side effects.
How do I get the results of my bone scan?
After the scan, the images are processed by a computer and read by a nuclear medicine radiologist. The radiologist then writes and sends a report to your provider who ordered the scan. Your provider will talk about these results with you.