Types of Radiation Therapy for Breast Cancer Treatment
Radiation can be used to treat some types of breast cancer. The type of radiation you get will depend on your treatment plan, the stage of your cancer, and other factors. Radiation can also be used if your cancer has spread to other parts of your body (bone, brain, etc.). This article will review some of the common ways that radiation therapy is used to treat breast cancer.
Whole Breast Radiation After Lumpectomy
After a lumpectomy (surgery to remove part of the breast), radiation is often given to the rest of your breast. This may not be done if you are older with a smaller, less aggressive tumor. This helps lessen the chance of cancer returning in the same place or in other areas of that breast. Radiation is most often given using external beam radiation. The radiation beams are angled so that they skim the chest wall but cover the whole breast. This type of radiation is usually delivered in daily treatments (5 days a week) over several weeks. An additional week may be used to give an extra dose (called a boost) to the original tumor location.
In some cases, after a lumpectomy, radiation will also be given to the lymph nodes under the arm (axillary). This depends on whether there was cancer found in the lymph nodes. Ask your radiation oncologist if you will need radiation to the axillary lymph nodes as part of your treatment.
Partial Breast Radiation After Lumpectomy
In some cases, after a lumpectomy, only the area of the surgical cavity (the spot where the tumor was removed) is treated with radiation, not the whole breast. If your cancer comes back in the same breast after treatment, it often comes back in or near the surgical cavity. By targeting this area, it limits the amount of radiation to the rest of the breast, chest wall, heart, and lungs. This method is called "accelerated partial breast irradiation" or APBI.
APBI is "accelerated" because you will get radiation two times a day for a shorter period of time than traditional external beam radiation. APBI can be delivered using external beam radiation, or through internal radiation (also called brachytherapy). For brachytherapy, a balloon or catheters are placed in the surgical cavity of the breast to deliver radiation right to the cavity. Brachytherapy can further limit the amount of radiation that hits normal structures like the heart, lungs, and chest wall.
Chest Wall and Lymph Node Radiation After Mastectomy
Not everyone who has a mastectomy (removal of the whole breast) will need radiation. If you had a mastectomy and there was no cancer in your lymph nodes, then radiation will likely be given to your entire chest wall including your surgery scar and areas where surgical drains were. To decide if you need this type of radiation, your provider looks at:
- The tumor size.
- The number of axillary lymph nodes with cancer cells.
- Tumor grade (appearance under the microscope).
- Invasion of lymphovascular spaces within the tumor.
- Surgical margins.
- Your age.
If these factors show you have a higher risk of cancer coming back at the chest wall (where the breast tissue previously attached) or in the nearby lymph nodes, radiation can lessen that risk. Treatment involves daily radiation (5 days a week) for many weeks, using external beam radiation therapy. In this case, the radiation is designed to skim the chest wall to avoid radiation exposure to the lung and, in left-sided cancers, the heart. If you had breast reconstruction, the radiation target will include the reconstructed breast.
Special Techniques to Reduce Side Effects
In some cases, it is hard to avoid the lung and/or heart during radiation. There are some options that can be used to lessen exposure to normal tissues. These options are:
- Treating with a deep inspiration breath-hold (DIBH) technique, which increases the distance between the heart and chest wall. This means holding your breath during certain parts of your treatment.
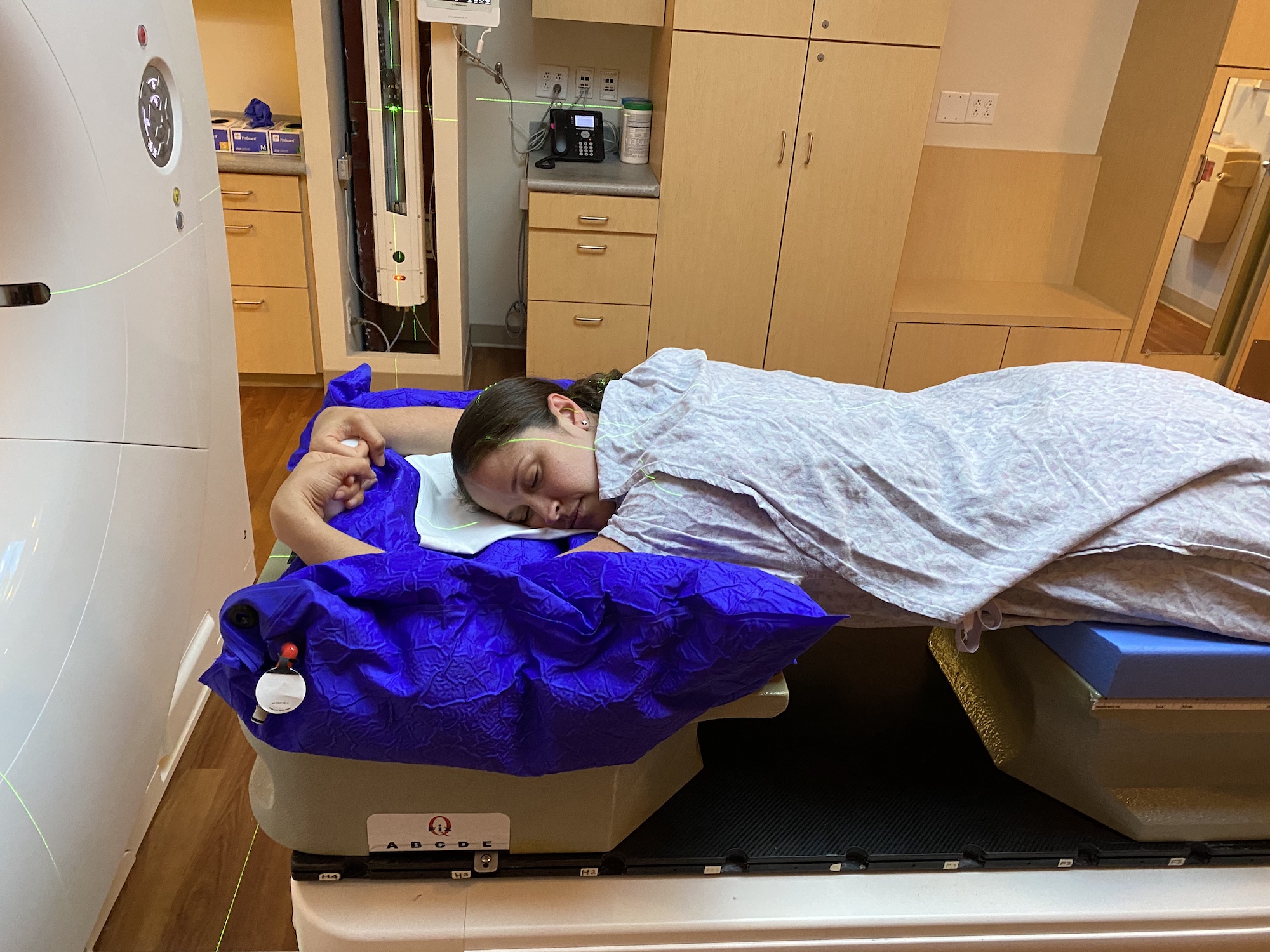
- Giving treatment in the "prone" position (lying on your stomach). This is most often used when treating the left breast, although it can be used for treatment of both the left and right breast. The prone position is helpful for the treatment of large, pendulous breasts. It allows gravity to pull the breast tissue down and away from the body sparing radiation to the heart, lung, and your other breast.
- Treating with proton radiation, instead of x-ray (photon) radiation. With proton therapy, the radiation can be delivered so that it stops before it gets to the heart and lung tissue.
There are many ways that breast cancer can be treated. Talk to your providers about what options are best for you.
After treatment, talk with your oncology team about a survivorship care plan, which can help you manage the transition to survivorship and learn about life after cancer. You can create your own survivorship care plan using the OncoLife Survivorship Care Plan. For more information about the long-term effects of radiation therapy for breast cancer, read our article, Survivorship: Late Effects after Radiation for Breast Cancer.