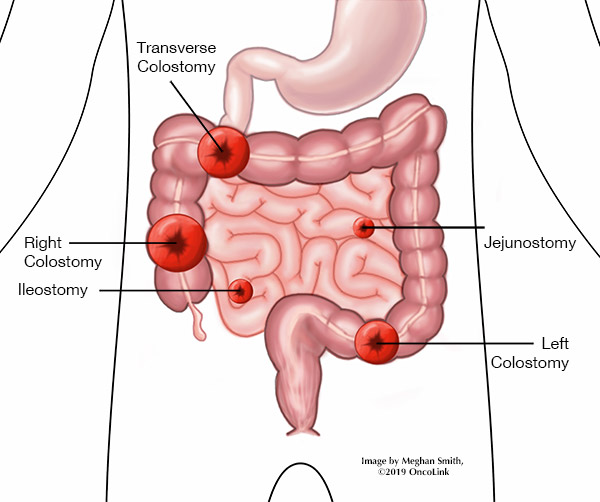
Surgical Procedures: Ileostomy
What is an ileostomy?
The ileum is the last part of the small intestine, before the colon. An ileostomy is a stoma (hole) in the belly that lets stool (bowel movements) pass through. Surgery is done to attach the ileum to the inside of the abdominal (belly) wall. This lets stool pass from the intestine, through the stoma, usually into a collection device outside of the body. The stoma can be seen on the outside of the belly. It should be pink to red in appearance, warm, and moist.
An ileostomy may be used to treat:
- Rectal cancer.
- Colon cancer.
- Benign inflammatory bowel conditions, such as Crohn’s disease and ulcerative colitis.
- Familial polyposis.
- Certain birth defects.
- Injury or trauma.
- Hirschprung’s disease.
What are the types of ileostomy?
Your healthcare provider will talk to you about the type of ileostomy you need, based on your situation and health status. An ileostomy can be temporary (short-term) or permanent (lifelong). This will depend on the type of surgery you are having.
- Permanent ileostomy may be needed after surgery to remove the large intestine, colon, rectum, or anus.
- Temporary ileostomy may be done if only part of the colon is removed and the rectum is left.
There are a few types of ileostomy:
- Standard Ileostomy (Brooks Ileostomy): Connects the ileum to the abdominal wall, exposing the intestinal mucosa to form a smooth external stoma. You will not be able to control your stool after this surgery, so you will need to wear an external bag (outside your body) for stool collection.
- Continent Ileostomy: There is no need for an external collection bag. You will be able to control your stool (continence) but your stool will need to be drained frequently with a catheter. To do this, your surgeon forms a pocket inside the abdomen (taking the place of the rectum) and puts a small external valve where the catheter will be placed to drain stool.
- Ileo-anal reservoir (J-pouch, S-pouch, W-pouch or pelvic pouch): Allows stool to pass from the anus. During this procedure, your surgeon makes a collection pouch from the ileum and rectum, which will collect the stool. The stool can then be passed from the anus.
What are the risks and side effects of having an ileostomy?
When you have an ileostomy, food leaves the body earlier in the digestion process. This will change how your stool looks when it leaves your body through the stoma. The stool you pass from the ileostomy will be liquid to pasty in consistency and contains digestive enzymes. Other risks and side effects of having an ileostomy may be:
- Infection.
- Bleeding.
- Blood clots.
- Damage or injury to nearby organs.
- Adhesion/scar tissue formation (An adhesion is scar tissue that joins 2 pieces of tissue that should not be joined. They are often painless and do not need treatment. Serious cases can cause a blockage in the bowel or limit blood flow).
- Bowel obstruction (This is a blockage in the bowel that can limit digestion or the removal of stool).
- Wound separation or issues with healing.
- Electrolyte changes in the body, most often with sodium and potassium.
- Diarrhea.
- Issues with the stoma, such as skin irritation, infection, and leaking.
- The feeling of needing to have a bowel movement called “phantom rectum.”
- Short bowel syndrome, which may lead to vitamin and nutrient absorption problems.
What is recovery like?
Recovery from an ileostomy will depend on the extent of the procedure you had. How long you stay in the hospital will depend on the procedure you had and how well you are recovering.
You will be told how to care for your surgical incisions/stoma and will be given any other instructions before leaving the hospital. Full instructions on caring for your stoma will be given to you by a specially trained stoma nurse/therapist.
Your care team will talk with you the medications you will be taking, such as those for pain, blood clot, infection, constipation prevention, management of diarrhea, and/or other conditions. They will also talk with you about the type of follow-up care you will need, like checking your blood electrolyte levels.
Your provider will tell you what you should and should not do when you go home. This will often include:
- Changes in activity level such as bending, lifting, and exercising.
- Not driving while taking pain medication.
- Returning to work in 2 to 4 weeks, depending on your job and work duties.
- Details about showering, submerging your surgical incisions in water, diet recommendations, sexual activity, and stoma care.
What will I need at home?
- Thermometer to check for fever (101°F, 38.3°C), which can be a sign of infection.
- Incision and stoma care supplies, often supplied by the hospital, your healthcare team, or the stoma nurse/therapist.
When should I call my provider?
- Signs of infection, including fever and redness, odor or drainage at the incision.
- Nausea, vomiting, bloating, or cramps lasting more than 2 hours.
- No ileostomy output for 4 to 6 hours with cramping and nausea.
- Leg swelling and/or sudden shortness of breath.
- Any new or worsening pain.
- A decrease in peeing.
- Blood in the ostomy pouch.
- Changes to the stoma, including retraction (pulling inward), changes in size or color, stoma blockage or bulging, bleeding, wounds, injury to the stoma, skin irritation/sores and/or watery stool for 5 or more hours.
How can I care for myself?
You may need a family member or friend to help you with your daily tasks until you are feeling better. It may take some time before your team tells you that it is ok to go back to your normal activity.
Be sure to take your medications as you are told to prevent pain, infection and/or constipation. Call your team with any new or worsening symptoms.
There are ways to manage constipation after your surgery. You can change your diet, drink more fluids, and take over-the-counter medications. Talk with your care team before taking any medications for constipation.
Taking deep breaths and resting can help manage pain, keep your lungs healthy after anesthesia, and promote good drainage of lymphatic fluid. Try to do deep breathing and relaxation exercises a few times a day in the first week, or when you notice you are extra tense.
- Example of a relaxation exercise: While sitting, close your eyes and take 5-10 slow deep breaths. Relax your muscles. Slowly roll your head and shoulders.
This article contains general information. Please be sure to talk to your care team about your specific plan and recovery.