Paracentesis
What is it?
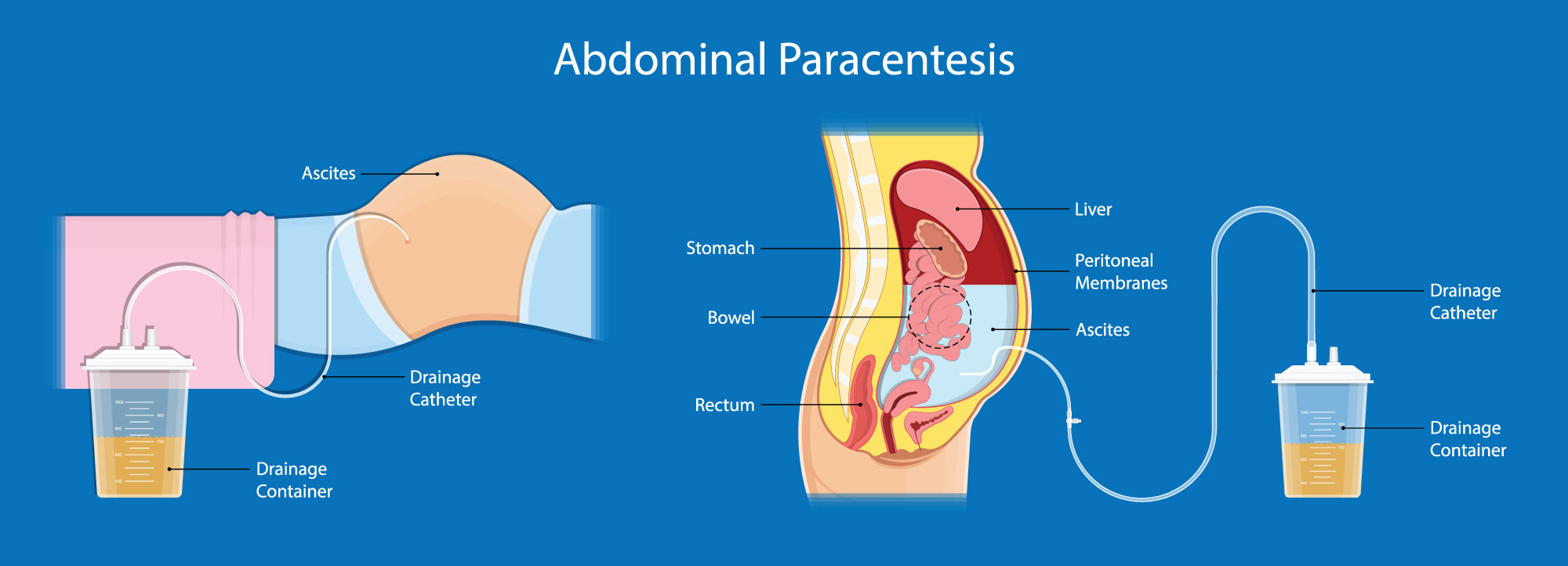
A paracentesis is a procedure done to remove fluid from the abdominal (belly) cavity using a needle. It is not normal to have fluid in this cavity, so any amount of fluid can cause you to have pain and a hard time breathing. The buildup of fluid in the abdomen is called ascites.
There are two reasons that a paracentesis may be done. These are:
- Diagnostic: Paracentesis is used to test the fluid and find the cause of the ascites. Ascites can be caused by infection, inflammation (swelling), trauma, cirrhosis of the liver, and cancer.
- Therapeutic: Paracentesis is done to relieve the symptoms and pain caused by ascites. In this case, the cause of the ascites is known.
Ascites is diagnosed based on your medical history, your physical exam, and diagnostic testing. Symptoms can include shortness of breath, discomfort, pain, and early satiety (feeling of fullness soon after you start eating). Your provider will palpate (touch with their hands) your stomach and may measure your abdominal girth (measurement around your stomach), and weight. You may have an abdominal x-ray, an ultrasound of your stomach, and an MRI or CT scan of your abdomen. These can all show a buildup of fluid.
Once your paracentesis is done and the fluid has been tested (if needed), your provider will let you know about the follow-up plan and further treatment options. Speak with your provider about any questions or concerns you may have.
How do you get ready for a paracentesis?
Paracentesis can be done either in a provider’s office or in the hospital. Your provider will tell you about the procedure and have you sign a consent form. Tell your provider about any medications you are taking, any bleeding disorders you have, allergies, or if you may be pregnant. You should not eat or drink anything for 12 hours before the procedure. You should use the bathroom before the start of the procedure.
A paracentesis takes about 10-30 minutes. You will be awake for the procedure. You should not have much pain during the paracentesis. You may be asked to put on a hospital gown. You may get pain and/or anti-anxiety medication before the procedure if needed.
How is it done?
- You will lie flat on your back or sit up. If you are not able to lie flat, you may have your head raised slightly. Once you are in a comfortable position, it is important to stay still.
- An ultrasound may be used to find the space where the fluid is easiest to reach. A cool or warm gel will be placed on the ultrasound probe, and you may feel slight pressure where the ultrasound is being used. This is not painful. Once your provider finds a good space to put in the needle, the spot will be marked.
- Next, the provider will clean the area where the needle will be put in. This will most likely feel cold. A drape may be put around the area where the needle will be placed.
- The area is then numbed. A small needle is placed into the skin to put in local anesthetic (numbing medication). You may feel burning or stinging for a short time from the numbing medication. Your provider will wait a few minutes to make sure the area is numb.
- Once the area is numb, your provider will put in a needle at the space that is marked. You may feel pressure or sharp pain for a short time as the needle is put in. If the pain does not go away, tell your provider. In some cases, a small incision (cut) may be made in the skin to insert the needle.
- The fluid will drain (come out) through the needle, or a tube connected to the needle, and into a container or test tube. It will be drained until the amount of fluid needed for testing is gathered or until your symptoms are relieved.
- Once the fluid is drained, the needle will be taken out, and a small bandage will be placed at the site. If an incision was made, the incision will be closed with 1-2 sutures and then covered with a bandage.
- Once the procedure is done, your vital signs may be checked, and your abdominal girth may be measured.
If you have had no side effects from the paracentesis, you can return to normal activity unless your provider tells you otherwise.
What are the risks?
Risks of paracentesis include:
- Leaking of fluid from the site where the needle was put in. This is normal and you may need to change the bandage a few times.
- Bleeding.
- Hypotension (low blood pressure). This can be a result of a large volume of fluid being taken out and is treated with intravenous (IV) fluids and sometimes a transfusion of blood products (red blood cells).
- Puncture of a blood vessel, bowel, or bladder. This is not common but may lead to the need for surgery.
- Infection. If the area appears infected (redness, tender or sore, pus or smelly drainage or if you get a fever), call your provider. Infection can be treated with antibiotics.
When should I call my care team?
It is normal for some clear fluid to drain from the site where the needle was put in, most often when a large amount of fluid was removed. You should call your care team if you have any signs of infection at the site. You should also call your provider if your abdomen increases in girth (feels more swollen or round), your pain does not get better with pain medication prescribed to you, or if you have chest pain, shortness of breath, blood in your urine, or uncontrolled bleeding from the site.