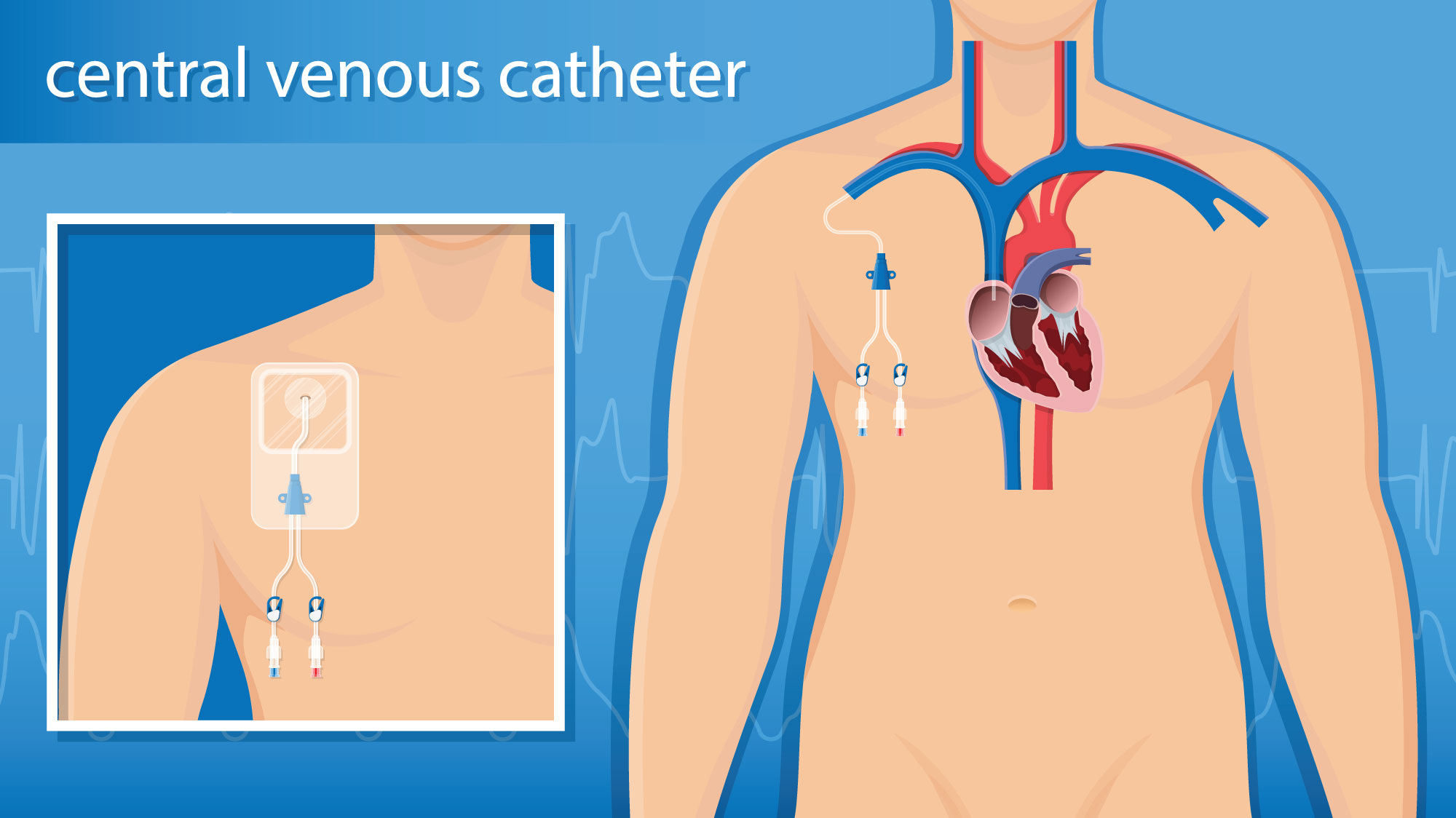
Hickman Line
A Hickman is a central line catheter that is placed on the right side of your chest wall. A Hickman line is a soft, small, long, hollow tube that is placed into a vein in the chest and ends in a larger vein just above your heart. A Hickman line is used long-term to access your veins and can be used to give chemotherapy, intravenous medications, nutrition, and to draw blood for labs.
How is it put in and used?
A Hickman line can be placed either as an in-patient or out-patient procedure. A sterile field is used to prevent infection. Numbing medication is given into your chest using a small needle. The care team will use an ultrasound machine to look at your veins. A small cut will be made and then the Hickman line will be placed into the right side of your chest. The site is covered by a dressing.
You will have one to three lumens (tubes) dangling from the site which will either be sutured in or a device that looks like a sticker will be used to keep it in place. The lumens are short, small tubes with caps at the end. The lumens are used to give medications or draw blood. When your provider uses these lumens it is sometimes called “accessing the Hickman line”. Once insertion of your Hickman line is done, an X-Ray will be taken to make sure your Hickman line is in the right place.
Possible Side Effects
There usually are no issues with placing a Hickman line. However, there is the risk of air embolism, phlebitis, blood clot, nerve irritation and injury and irritation to the heart muscles resulting in arrhythmia.
Other issues may arise after placement, while the Hickman is in use. A central line is a direct portal into your veins. The most common issue with a central line is an infection, blood clot, or a clot in the catheter (occlusion). Having a catheter puts you at a higher risk of getting a blood clot in the vein where the catheter is located. An occlusion is a blockage in your line, which makes the catheter unusable. Each day you should look at your central line to check for any changes to the dressing, the insertion site, and the lumens. Make sure your dressing is intact and not wet or dirty. Signs of infection may be seen at the insertion site and include redness, swelling, drainage, bruising, and bleeding. Signs of a blood clot can include swelling around the area.
How do I care for my catheter?
- Hands should be washed by anyone touching or accessing the Hickman line. Prior to touching the Hickman line hands should be washed and gloves put on. After touching the Hickman line, gloves should be removed and hands once again washed.
- A dressing will be put over the Hickman line insertion area. This keeps the area clean and helps keep the Hickman line from coming out. The dressing should be changed at least once a week, or if it becomes wet or dirty. Use a plastic cover or sleeve to cover your Hickman line while bathing. Never use scissors to cut away a dressing.
- The Hickman line must be flushed on a regular basis to prevent it from becoming occluded. Flushing entails attaching a syringe filled with normal saline solution and administering the fluid into the Hickman line through the cap. With some Hickman lines, a medication called heparin is also used which prevents clotting. Usually, the Hickman line needs to be flushed every day.
- Assess your Hickman line each day to monitor for signs of infection and loosening or contamination of the dressing.
- Do not pull on the Hickman line. Take care to secure the lumens against your skin to prevent accidentally pulling out your Hickman line.
- When the Hickman line is no longer needed, it may be removed by your provider.
Your care team will show you or a family member how to change the dressing or flush the line if it is necessary for this to be done when you are at home.
When to contact your care team
Daily monitoring of your catheter is necessary so that you can identify any changes. If you notice any redness, pain, discharge, or swelling at the site of insertion contact your provider immediately. You also want to contact your provider if flushing of the line is difficult, the lumens are cut or break, you have any pain with use of the Hickman line, or the Hickman line has become dislodged from your chest.
References
Camp-Sorrell D. Clinical dilemmas: vascular access devices. Seminars in Oncology Nursing. 2007:23(3)232-239.
Central lines (skin-tunnelled venous catheters). [Internet]. MacMillian Cancer Support. Available at: https://www.macmillan.org.uk/information-and-support/treating/chemotherapy/being-treated-with-chemotherapy/central-lines.html