Radiation Therapy Thermoplastic Mask
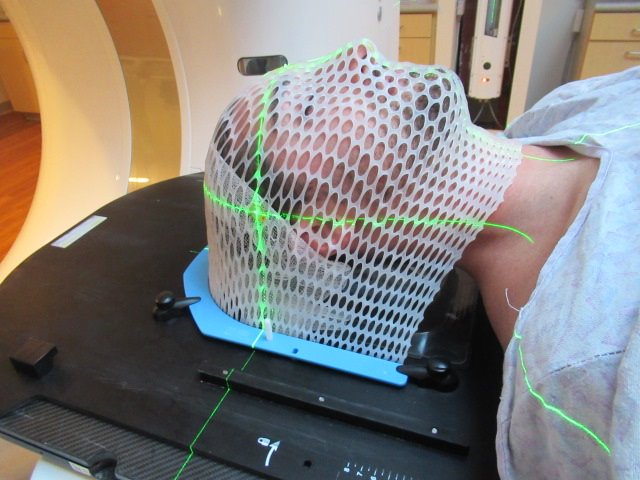
If you need radiation therapy to your head and neck or brain, you will likely have to get a thermoplastic mask made for your treatment. Thermoplastic masks are made of a plastic material that looks like mesh.
The mask helps you stay still during treatment for accurate delivery of the radiation beam. The mask will be made at the time of your CT simulation. You will wear it every day for treatment. You will not be able to talk when you have the mask on. You can communicate with the therapists using your hands while you have the mask on. You can give a thumbs up or thumbs down to answer simple questions that the therapists may ask. If you need the therapists during treatment, you can raise or wave your hand and they will come into the treatment room to check on you.
What personal items need to be removed before making the mask?
You will be asked to take off any removable items that are in the treatment area. This could be things like:
- Dental work.
- Wigs.
- Hairpieces.
- Head scarfs.
- Bobby pins.
What is the mask-making process?
The mask-making process can differ based on the area of your head and neck or brain the treatment will be focused on and if other devices will be used with the mask. Generally, the process is similar and will follow these steps:
- You will be asked to put on a gown for this procedure and for your daily radiation treatments.
- You will be lying on your back and you will want to continue breathing normally.
- The mask starts off hard, it is then placed in a warm water bath and becomes pliable (flexible) after about 3-4 minutes. Gauze, stockinette, or other material may be placed over your head so the mask does not stick to your hair.
- The mask will be taken out of the water bath, excess water is removed, and it is gently stretched over your face. The mask will feel warm and wet, like a hot towel that would be used during a facial.
- The mask is then secured to the table using clips.
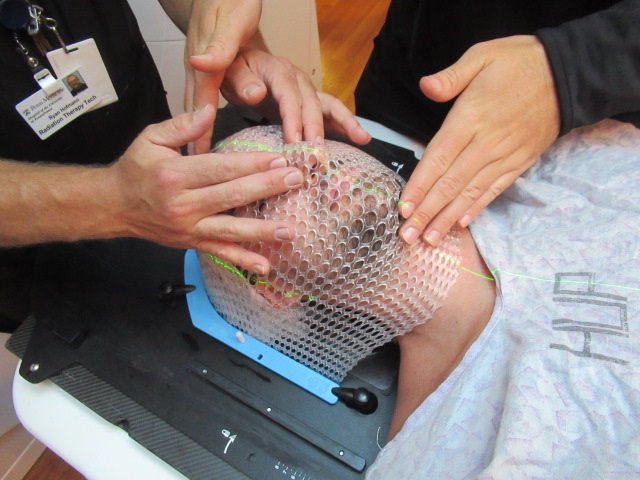
- The therapists will use their fingers to mold the mask so that it takes the shape of your head, face, eyes, ears, and throat.
- The holes in the mesh mask will make it easy for you to breathe and see.
- You will want to stay still while the mask is cooling. The mask takes about 10 minutes to completely cool and harden.
- After the mask has hardened you will get a CT scan in the position you are in, with the mask on. The mask-making and CT simulation process takes about 30-45 minutes.
Once your mask is made, do not make any major hairstyle changes, including changes to your facial hair.
What other immobilization devices are used with the mask?
You may be asked to use a bite block or mouthpiece with your mask. There are many types of bite blocks, but they all do the same thing. It is placed inside your mouth to hold your mouth and jaw in the same position. It can also be used to help reduce side effects, by depressing your tongue.
- Bite blocks are soft pieces of dental wax or plastic that are placed in your mouth. You will be asked to bite it for a few minutes until it hardens.
- A mouthpiece is like a mouthguard used in sports.
If your provider wants you to use the bite block or mouthpiece it will be placed during the simulation and used every day for treatment with your mask.
Why is the mask important?
The mask is important for your treatment because it holds your head and neck stationary (still) and in the exact position needed for treatment. This helps make sure that your treatment is accurate and as effective as possible. In most cases, after your treatment is complete you can take your mask home with you.