Surgical Procedures: Sentinel Lymph Node Biopsy
Also known as: Sentinel node biopsy, SLN biopsy
What is a lymph node?
Lymph nodes are part of your lymph system. These nodes have cells in them that help clear out bacteria and other things that shouldn’t be in your body. Cancer cells can spread through your lymph system to other parts of your body. Because of this, lymph nodes are one of the earliest sites of spread (metastasis) for some cancers.
A sentinel lymph node(s) is the lymph node(s) where cancer cells spread first from the primary (original) tumor.
What is a sentinel lymph node biopsy?
A sentinel lymph node (SLN) biopsy is surgery done to remove one or a few of these lymph nodes. This is done to help see if cancer has spread to other parts of your body.
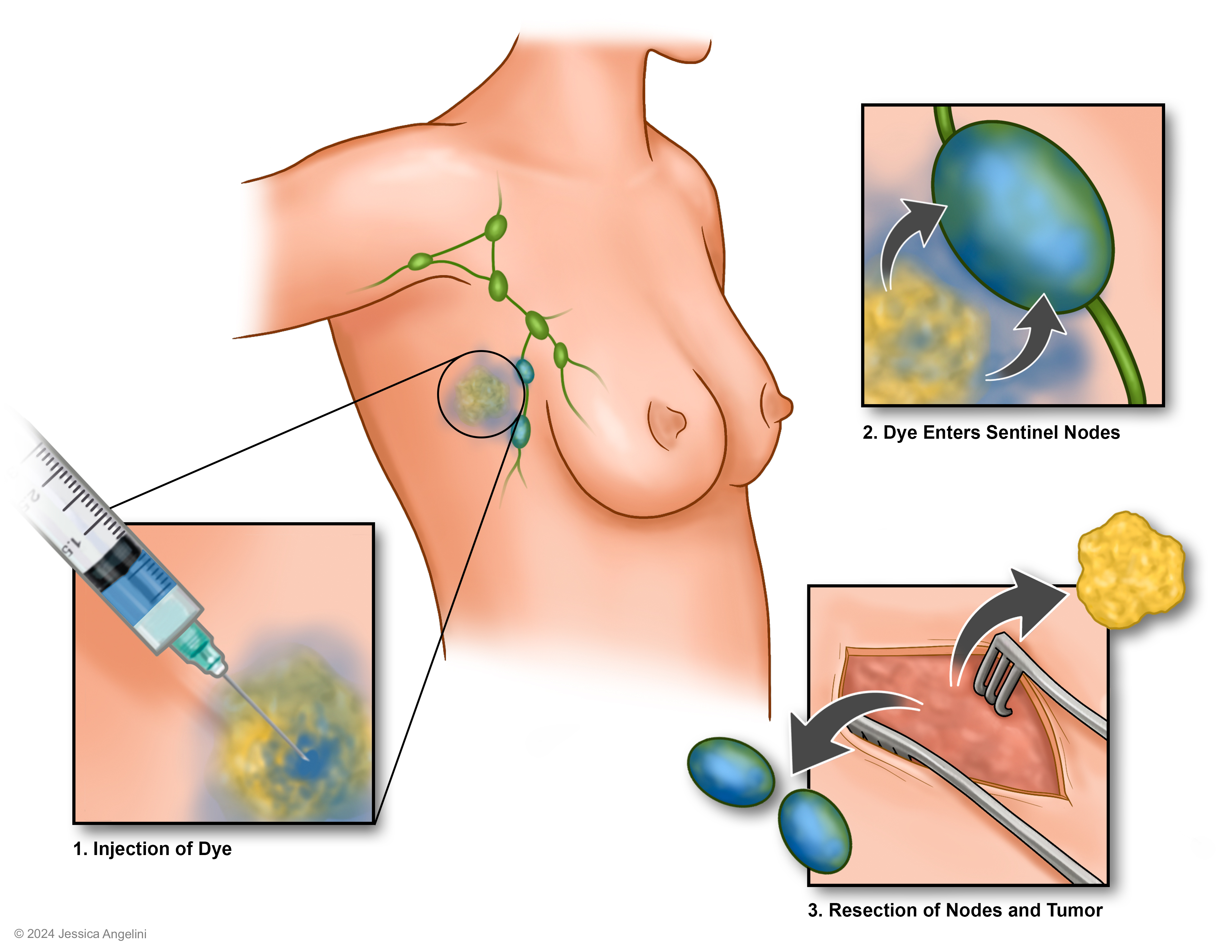
How is it done?
- You will have a blue dye and/or a radioisotope (a nuclear medicine dye) injected into the area of your tumor. This may be done in the nuclear medicine department. It can be done a few hours to up to a day before the biopsy or in the operating room right before the biopsy. Your care team will tell you how the dye will be given.
- Once the dye(s) is injected, your lymph system picks up the dye near the tumor and it travels to nearby lymph node(s).
- In the operating room, you will be given anesthesia to put you to sleep for the biopsy. You will not remember the procedure.
- An incision (cut) is made, and the surgeon finds the lymph nodes with dye.
- The nodes that pick up the dye are the sentinel lymph nodes. They are removed and tested for cancer cells.
During this surgery, only the sentinel nodes are removed. The rest of the nodes are left alone. This lowers the chance of getting a chronic swelling problem called lymphedema.
Will I stay overnight?
No. This is often done as an outpatient or "same-day" surgery. If you are having the SLN biopsy done at the same time as another surgery, you may need to stay overnight.
Will I need more surgery?
If cancer is found in one or more sentinel lymph nodes, you and your provider will talk about a treatment plan.
What is recovery like?
You and your provider will talk about what your recovery will be like. You will be up and moving the day of or the day after surgery. There will be some changes to your normal schedule and exercise routine in the first week or so. After surgery, you could have side effects, like:
- Blue urine and greenish-colored stool for 24 to 48 hours after the injection of blue dye. You are not radioactive after receiving the radioactive tracer.
- Pain, numbness, and/or sensitivity near the incision or in the limb where the surgery was done.
- You could get a seroma. A seroma is when lymph fluid builds up instead of draining as it should. It is not a worry, but it can be uncomfortable. Most go away on their own but may need to be drained in the office with a needle.
- Lymphedema is chronic swelling in a body part. There is a low risk of getting lymphedema after this procedure, but this risk is life-long.
How can I prevent infection?
Getting an infection after surgery is not common, but you can help prevent infection by:
- Taking a shower the night before surgery and washing your body with soap and water.
- On the second day after surgery, make sure to shower and clean the incision with soap and water. Pat dry and do not rub the incision. Do this every day, or at least every other day, to keep the incision site clean.
- Do not soak in a tub or go swimming. Your incision should not go underwater.
- Wash your hands before and after touching the incision or changing the dressing.
What will I need at home?
- 4 x 4 gauze pads and 1-inch paper tape to cover the incision if it is leaking.
- Clean, comfy pillow(s) to put under your arm or leg while sitting or to help with positioning at night.
How do I care for the incision?
Your provider will tell you when to remove your bandage. After it is removed, you may shower, but do not scrub the incision. To dry, gently pat the incision with a clean towel. Do not use lotions, powders, or deodorant on or near the incision during the first 1 to 2 weeks until it is fully healed.
Often, sutures that dissolve (break down on their own) are used. This type of suture doesn’t need to be removed. On the outside, some surgeons use surgical glue over the incision to give more protection. Others use paper tape called steri-strips while others use nothing. Both glue and steri-strips can get wet in the shower when you are cleared to do so.
How can I care for myself?
You may need a family member or friend to help you with your daily tasks until you are feeling better. It may take some time before your team tells you that it is ok to go back to your normal activity.
Be sure to take your prescribed medications as directed to prevent pain, infection, and/or constipation. Call your team with any new or worsening symptoms.
There are ways to manage constipation after your surgery. You can change your diet, drink more fluids, and take over-the-counter medications. Talk with your care team before taking any medications for constipation.
Taking deep breaths and resting can help manage pain, keep your lungs healthy after anesthesia, and promote good drainage of lymphatic fluid. Try to do deep breathing and relaxation exercises a few times a day in the first week, or when you notice you are extra tense.
- Example of a relaxation exercise: While sitting, close your eyes and take 5-10 slow deep breaths. Relax your muscles. Slowly roll your head and shoulders.
This article contains general information. Please be sure to talk to your care team about your specific plan and recovery.