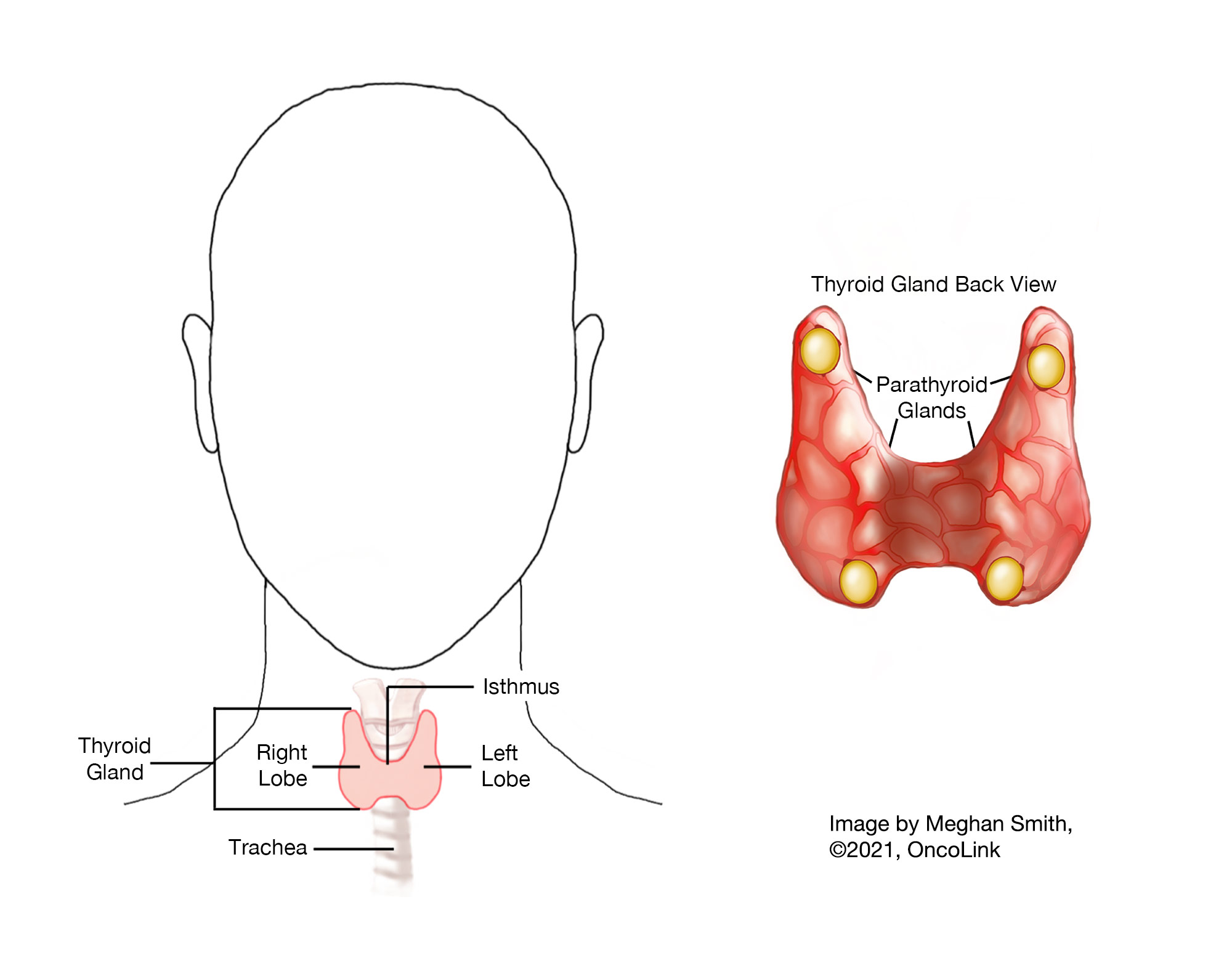
Parathyroid Cancer: Staging and Treatment
What is staging for cancer?
Staging is the process of learning how much cancer is in your body and where it is. Tests like blood tests, a physical exam of your neck, a Sestamibi/SPECT scan (a type of CT scan and a biopsy may be done to help learn about your parathyroid cancer. Your providers need to know about your cancer and your health so that they can plan the best treatment for you.
How is parathyroid cancer staged?
Unlike other cancers, there is no standard staging system for parathyroid cancer. After testing is done, your team may refer to the cancer as:
- Localized (kept to one area), or
- Metastatic (spread to areas away from the original tumor).
How is parathyroid cancer treated?
Treatment for parathyroid cancer depends on many things, like your cancer stage, age, overall health, and testing results. Your treatment may include some or all of the fo
llowing:
- Surgery.
- Chemotherapy.
- Targeted Therapy.
- Radiation Therapy.
- Clinical Trials.
Surgery
Surgery is the main treatment for parathyroid cancer. There are three types of surgery that may be used:
- En bloc resection: A surgery to remove the whole abnormal parathyroid gland and the capsule around it. In some cases, lymph nodes, half of the thyroid gland on the same side of body as the cancer, muscle, tissue, and nerves in the neck are also removed.
- Tumor debulking: Sometimes the whole tumor cannot be removed. Tumor debulking removes as much of the tumor as possible.
- If the cancer has spread to other areas of the body (metastasized), a surgical procedure may be done to remove the tumors in other organs in the body, such as the lung.
Your team will talk to you about your best option for surgical treatment. Surgery for parathyroid cancer can sometimes affect the nerves of the vocal cords. If damage to the vocal cords happens, you may need treatments to help with speech problems.
Radiation Therapy
Radiation is the use of high-energy x-rays to kill the tumor. The type of radiation used for parathyroid tumors is called external beam radiation therapy. Radiation can be used to treat parathyroid cancer that is localized, metastatic, or recurrent (came back after treatment). You and your care team will decide if radiation is needed for the treatment of your parathyroid cancer.
Chemotherapy
Chemotherapy are medications that travel through the bloodstream and throughout the body to kill cancer cells. Chemotherapy is not often used to treat parathyroid cancer because it is not very effective. In some cases of metastatic and recurrent parathyroid cancer, chemotherapy is used when surgery can’t be done. There is no standard chemotherapy regimen used for parathyroid cancer. The following chemotherapy medications may be used, either alone or in combination, to treat parathyroid cancers: dacarbazine (DTIC), 5-fluorouracil, cyclophosphamide, methotrexate, doxorubicin, and lomustine.
Clinical Trials
You may be offered a clinical trial as part of your treatment plan. To find out more about current clinical trials, visit the OncoLink Clinical Trials Matching Services.
Making Treatment Decisions
Your care team will make sure you are included in choosing your treatment plan. This can be overwhelming as you may be given a few options to choose from. It feels like an emergency, but you can take a few weeks to meet with different providers and think about your options and what is best for you. This is a personal decision. Friends and family can help you talk through the options and the pros and cons of each, but they cannot make the decision for you. You need to be comfortable with your decision – this will help you move on to the next steps. If you ever have any questions or concerns, be sure to call your team.
You can learn more about parathyroid cancer at OncoLink.org
References
Canadian Cancer Society. Parathyroid Cancer. 2021.https://www.cancer.ca/en/cancer-information/cancer-type/parathyroid/treatment/?region=on
Cancer.Net. Parathyroid Cancer. 2021. https://www.cancer.net/cancer-types/parathyroid-cancer/introduction
Munson ND, Foote RL, Northcutt RC, Tiegs RD, Fitzpatrick LA, Grant CS, van Heerden JA, Thompson GB, Lloyd RV. Parathyroid carcinoma: is there a role for adjuvant radiation therapy? Cancer. 2003 Dec 1;98(11):2378-84. doi: 10.1002/cncr.11819. PMID: 14635072
National Cancer Institute. Parathyroid Cancer Treatment Professional Version. 2021. https://www.cancer.gov/types/parathyroid/hp/parathyroid-treatment-pdq#_108_toc
National Cancer Institute. Parathyroid Cancer Treatment Patient Version. 2021. https://www.cancer.gov/types/parathyroid/patient/parathyroid-treatment-pdq
NCCN Guidelines Version 2.2020 Neuroendocrine and Adrenal Tumors. 2021. https://www.nccn.org/professionals/physician_gls/pdf/neuroendocrine.pdf (log in required).