Surgical Procedures: Cholecystectomy
What is a cholecystectomy and how is it done?
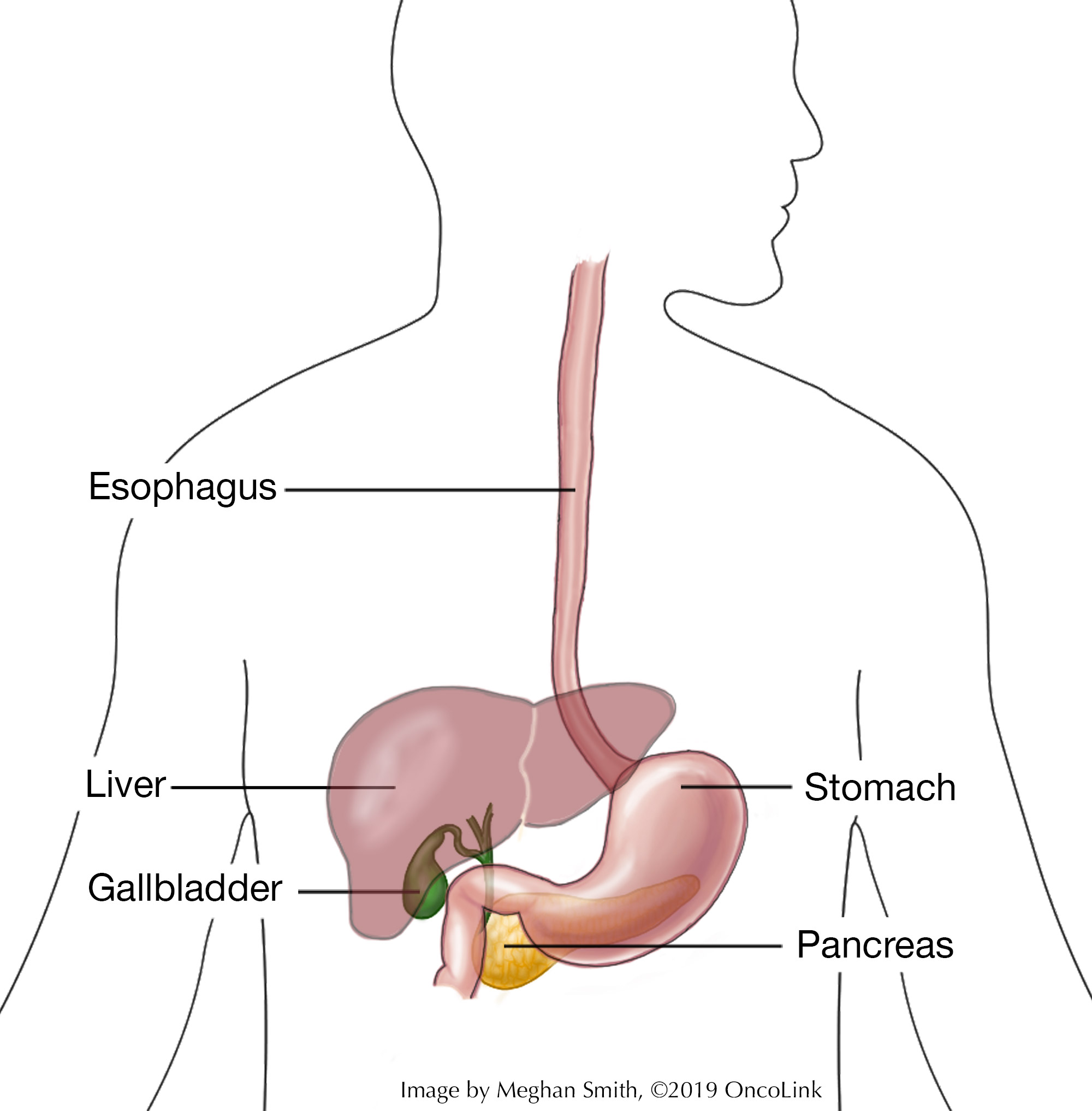
A cholecystectomy is a surgery that removes the gallbladder. The gallbladder is found in the right upper part of the belly, under the liver. Bile is a fluid that helps digest fat. It is made by the liver and stored in the gallbladder. Bile is then released through the common bile duct when it is needed. The common bile duct is what connects the gallbladder and liver to the first part of the small intestine.
A cholecystectomy may be used to treat some cases of:
- Gallbladder cancer.
- Cholelithiasis (gallstones within the gallbladder).
- Choledocholithiasis (gallstones within the bile duct).
- Cholecystitis (inflammation of the gallbladder).
- Pancreatitis (inflammation of the pancreas).
A cholecystectomy can be done in a few different ways, such as:
- Simple Cholecystectomy: The gallbladder and some of the surrounding tissue are removed. This is used in cases of early-stage cancers or non-cancerous issues. The procedure can be done open or laparoscopically:
- Open Cholecystectomy: The gallbladder is removed through a large (about 6 inch) abdominal incision (cut). This is not the preferred method when a patient has cancer or cancer is suspected. Most patients will have an extended cholecystectomy in these cases (see below).
- Laparoscopic Cholecystectomy: Many small incisions (cuts) are made in the belly. A laparoscope (lighted tube), placed through the incisions, is used to remove the gallbladder. This method is not used when gallbladder cancer is known or suspected.
- Extended (Radical) Cholecystectomy: Often, an extended cholecystectomy is used for patients with gallbladder cancer to decrease the risk of the cancer coming back. This is when the gallbladder, part of the liver, and many lymph nodes are taken out. In some cases, any of these are removed:
- A large portion of the liver (also called wedge resection).
- A liver lobe (also called hepatic lobectomy).
- The common bile duct.
- Pancreas.
- Duodenum.
- Certain ligaments, lymph nodes, and other areas where the cancer may be.
What are the risks associated with undergoing a cholecystectomy?
As with any surgery, there are risks and possible side effects. These can be:
- Reaction to anesthesia (anesthesia is the medication you are given to help you sleep through the surgery, to not remember it, and to manage pain. Reactions can be wheezing, rash, swelling, and low blood pressure).
- Bleeding.
- Infection.
- Blood clots.
- Scarring and/or numbness at the incision.
- Incisional hernia (this is when tissue in the belly pushes through the muscle. It can look like a lump and can be painful or tender when touched).
- Pneumonia.
- Injury to the bile duct, small intestine, and/or liver.
What is recovery like?
Recovery from a cholecystectomy is based on the type of procedure you have had. At times, a hospital stay is needed for 2 to 3 days.
You will be told how to care for your incisions, and any other instructions before leaving the hospital.
Your medical team will discuss with you the medications you will be taking, such as those for pain, blood clot, infection, constipation prevention, and/or other conditions.
Your healthcare provider will discuss your activity restrictions.
For those who have had a laparoscopic procedure:
- Take pain medication as told.
- Do not drive while taking narcotic medication.
- Follow the instructions you have been given for showering.
- Ask your provider when it is safe to go back to work.
- Your healthcare team will provide you with instructions on how to care for your incision.
- Do not use antibiotics or creams on the scar unless you have been told to do so.
For those who have had an open procedure:
- Avoid heavy lifting until told to do so by your care team.
- No tub bathing, hot tubs, or swimming.
- Take pain medications as prescribed.
- Consider placing a pillow over the surgical incision when coughing/sneezing to add incisional support and reduce pain.
- Follow the instructions you have been given for the care of your incision.
What will I need at home?
- Thermometer to check for fever, which can be a sign of infection.
- Loose-fitting clothes.
- Incisional care items, often supplied by the hospital/physician's office.
Call your healthcare team if you experience:
- Fever. Your team will tell you at what temperature you should call.
- Chills.
- Worsening swelling/bloating of the belly.
- Any new or worsening pain.
- Drainage, bleeding, and/or warmth at the incision.
- Difficulty breathing.
- Persistent cough, nausea, and/or vomiting.
- Inability to eat or drink.
- Yellowing of the skin or the whites of the eyes (jaundice).
- Gray bowel movements.
How can I care for myself?
You may need a family member or friend to help you with your daily tasks until you are feeling better. It may take some time before your team tells you that you can go back to your normal activity.
Be sure to take your prescribed medications as directed to prevent pain, infection and/or constipation. Call your team with any new or worsening symptoms.
There are ways to manage constipation after your surgery. You can change your diet, drink more fluids, and take over-the-counter medications. Talk with your care team before taking any medications for constipation.
Taking deep breaths and resting can help manage pain, keep your lungs healthy after anesthesia, and promote good drainage of lymphatic fluid. Try to do deep breathing and relaxation exercises a few times a day in the first week, or when you notice you are extra tense.
- Example of a relaxation exercise: While sitting, close your eyes and take 5-10 slow deep breaths. Relax your muscles. Slowly roll your head and shoulders.
This article contains general information. Please be sure to talk to your care team about your specific plan and recovery.