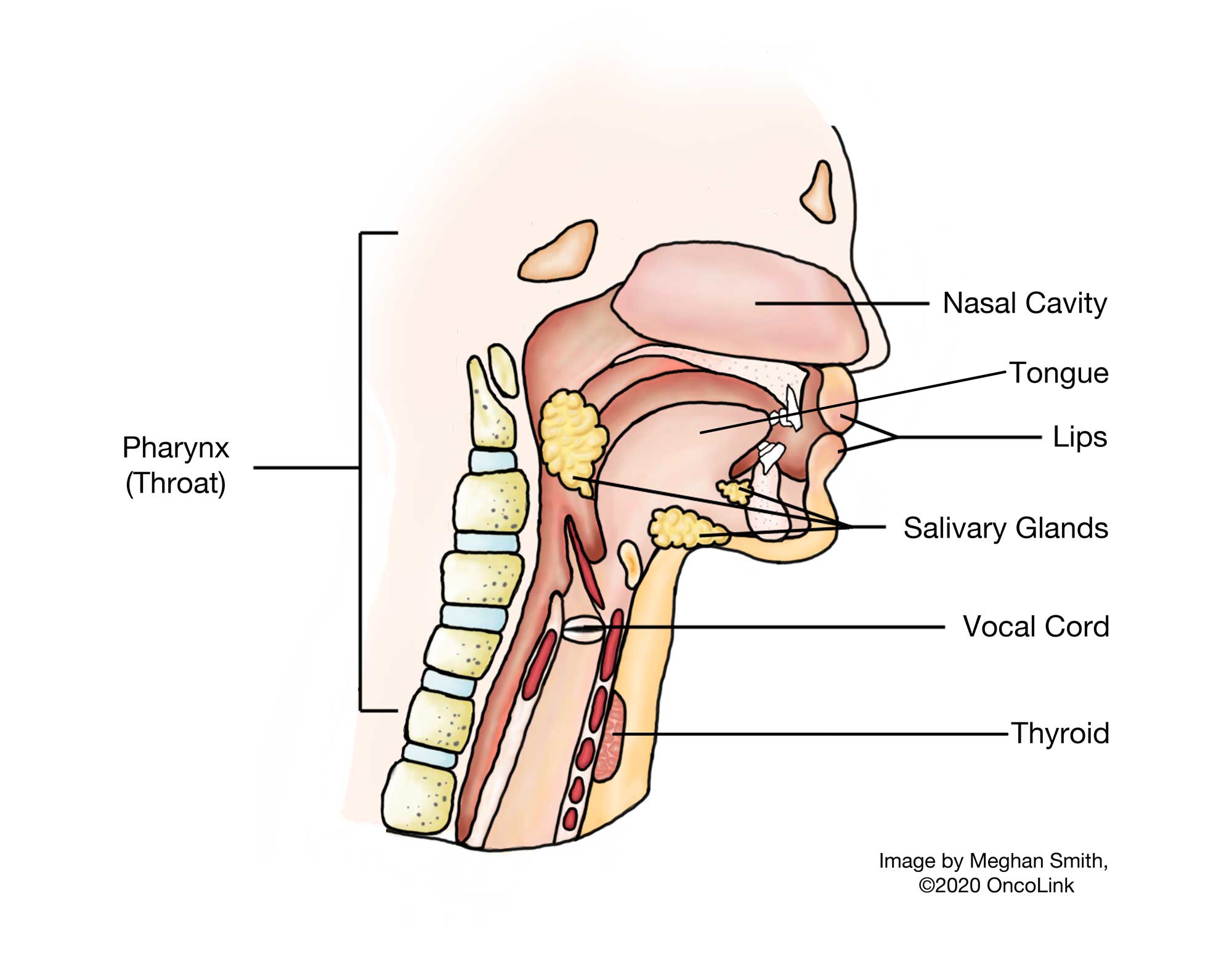
Hypopharyngeal (Lower Throat) Cancer: Staging and Treatment
What is staging for cancer?
Staging is the process of learning how much cancer is in your body and where it is. Tests like biopsy, laryngoscopy, bone scan, PET scan, CT, and MRI may be done to help stage your cancer. Your providers need to know about your cancer and your health so that they can plan the best treatment for you.
Cancer staging looks at the size of the tumor and where it is, and if it has spread to other areas of your body. The staging system for hypopharyngeal cancer is called the “TNM system.” It has three parts:
- T-Describes the size/location/extent of the "primary" tumor.
- N-Describes if the cancer has spread to the lymph nodes.
- M-Describes if the cancer has spread to other organs (called metastases).
Your healthcare provider will use the results of the tests you had to figure out your TNM result and combine these to get a stage from 0 (zero) to IV (four).
How is hypopharyngeal cancer staged?
Staging for cancer of the hypopharynx (lower throat) is based on:
- The size of your tumor seen on imaging tests and what is found after surgery (if you have had surgery).
- If your lymph nodes have cancer cells in them.
- If the cancer has spread to other parts of your body (metastasis).
The staging system is very complex. Below is a summary of the staging. Talk to your provider about the stage of your cancer.
Stage 0 (Tis, N0, M0): The tumor is only in the top layer of cells lining the inside of the hypopharynx and has not grown any deeper (Tis). The cancer has not spread to nearby lymph nodes (N0) or to distant parts of the body (M0).
Stage I (T1, N0, M0): The tumor has grown deeper, but it is only in one part of the hypopharynx, and it is no more than 2 centimeters (cm) (T1). The cancer has not spread to nearby lymph nodes (N0) or to distant parts of the body (M0).
Stage II (T2, N0, M0): The tumor has grown into more than one part of the hypopharynx, OR it has grown into a nearby area, OR it is 2 to 4 cm and has not affected the vocal cords (T2). The cancer has not spread to nearby lymph nodes (N0) or to distant parts of the body (M0).
Stage III (T3, N0, M0): The tumor is bigger than 4 cm, OR the tumor is affecting the vocal cords, OR the tumor has grown into the esophagus (T3). The cancer has not spread to nearby lymph nodes (N0) or to distant parts of the body (M0); OR (T1-T3, N1, M0): The tumor can be any size and may have grown into structures outside the hypopharynx, and it may have affected a vocal cord (T1 to T3). The cancer has spread to a single lymph node on the same side of the neck as the tumor, and it is less than 3 cm in size (N1). The cancer has not spread to distant parts of the body (M0).
Stage IVA (T4a, N0-N1, M0): The tumor has grown into the thyroid or cricoid cartilage, the hyoid bone, the thyroid gland, or nearby areas of muscle or fat. This is also known as moderately advanced local disease (T4a). The cancer has not spread to nearby lymph nodes (N0), or it has spread to a single lymph node on the same side of the neck as the tumor, which is less than 3 cm in size (N1). The cancer has not spread to distant parts of the body (M0); OR (T1-T4a, N2, M0): The tumor can be any size and might or might not have grown into structures outside the hypopharynx (as far as moderately advanced disease), and it might or might not have affected a vocal cord (T1 to T4a). The cancer is N2 if:
- It has spread to a single lymph node on the same side of the neck as the tumor, which is 3 to 6 cm in size, OR
- It has spread to more than one lymph node on the same side of the neck as the tumor, which are all less than 6cm, OR
- It has spread to at least one lymph node on the other side of the neck, which are all less than 6cm.
The cancer has not spread to distant parts of the body (M0).
Stage IVB (T4B, Any N, M0): The tumor is growing into the area in front of the spine in the neck, goes around a carotid artery, or is growing down into the space between the lungs. This is called very advanced local disease (T4b). The cancer may have spread to nearby lymph nodes (any N). It has not spread to distant parts of the body (M0); OR (Any T, N3, M0): The tumor can be any size and may have grown into structures outside the hypopharynx, and it may have affected a vocal cord (any T). The cancer has spread to at least one lymph node that is larger than 6 cm across, OR it has spread to a lymph node and then grown outside of the lymph node (N3). It has not spread to distant parts of the body (M0).
Stage IVC (Any T, Any N, M1): The tumor can be any size and may have grown into structures outside the hypopharynx, and it may have affected a vocal cord (any T). The cancer may have spread to nearby lymph nodes (any N). The cancer has spread to distant parts of the body (M1).
How is hypopharyngeal cancer treated?
Treatment for hypopharyngeal cancer depends on many things, like your cancer stage, age, overall health, and testing results. There are steps to take before treatment starts for any kind of head and neck cancer:
- Multidisciplinary treatment is very important. This means you will have providers from many different specialties involved in your care. Many of these providers will see you before you start cancer treatment during visits called consultations. They will work together and with you to make a plan to treat your cancer.
- If you smoke, quit as soon as possible. Smoking may lessen how well your cancer medications work and can make side effects worse.
Your treatment may include some or all the following:
- Surgery
- Radiation Therapy.
- Chemotherapy.
- Targeted Therapy.
- Immunotherapy.
- Supportive/Palliative Treatment.
- Clinical Trials.
Surgery
The type of surgery you have depends on where your tumor is, the stage, and your overall health. Surgery for head and neck cancer can be challenging, including the removal of tissue and bone and the use of plastic surgery to rebuild facial features to improve how they work and look.
The goal of surgery is to remove as much of the cancer as possible while sparing healthy tissue or organs near the tumor. There are a few surgeries that may be used to treat cancer of the hypopharynx:
- Vocal Cord Stripping: The top layers of tissue on the vocal cords are stripped away using a long surgical tool. This is used to biopsy or treat stage 0 cancer. After you recover, your normal speaking voice often returns.
- Cordectomy: Either part or all of your vocal cords are removed. How much this affects your ability to talk is based on how much of the vocal cord is removed. If only part of the vocal cord is removed, your voice may be hoarse. If both cords are removed, you will not be able to speak normally.
- Laryngectomy: There are many types of laryngectomies:
- Partial Laryngectomy: This procedure is used in smaller cancers where only part of the larynx is removed. There are two types:
- Supraglottic laryngectomy: The part of the larynx above the vocal cords, known as the supraglottis, is removed. You will be able to speak normally after surgery.
- Hemilaryngectomy: Used in smaller tumors of the vocal cords, involves the removal of one side of the larynx (and one vocal cord). Because one vocal cord remains, you will still be able to talk after, but your voice may change.
- Total Laryngectomy: Used in advanced cancers, the whole larynx is removed. The windpipe (trachea) will be brought up through the skin on the front of the neck making a hole (stoma) that you will now breathe through, rather than through your nose or mouth. This is known as a tracheostomy. You will not be able to speak normally. After recovery from the surgery, you should be able to swallow normally.
- Partial Laryngectomy: This procedure is used in smaller cancers where only part of the larynx is removed. There are two types:
- Laser Surgery: In laser surgery, an endoscope is placed into your mouth and down into your throat to find and vaporize or cut out (excise) the tumor using the laser that is on the tip of the endoscope. If this technique is used to remove part of the vocal cord, it can cause a hoarse voice.
- Lymph Node Dissection: If your provider thinks that the cancer has spread to the lymph nodes, they may choose to do a lymph node dissection or removal. There are several types of dissections, which can range from the removal of one or a few lymph nodes to the removal of nodes, nerves, and muscle. Your surgeon will determine the extent of dissection needed based on the size and location of the original tumor and if the nodes were enlarged on previous imaging tests.
Some patients may need a partial or full pharyngectomy, which is the removal of the throat. If the cancer has affected your thyroid, you may need a thyroidectomy.
Talk with your care team about your surgical options, any concerns about your body image and function, what you will need to do to heal after surgery, and side effects that you may have. You will likely need to see providers after surgery to help you with your speech and dietitians to help make sure you are getting enough nutrition.
Radiation Therapy
Radiation therapy is the use of high-energy x-rays to kill cancer cells. Radiation for hypopharynx cancer can be used:
- Alone.
- With chemotherapy at the same time (called chemoradiation).
- After chemotherapy.
- For palliative treatment (to ease symptoms).
- If the cancer has come back (recurrence).
There are two main types of radiation used to treat hypopharynx cancer:
- External radiation therapy: A beam of radiation from outside of the body is aimed into the body. It may also be called x-ray therapy, 3D conformal radiation, intensity-modulated radiation therapy (IMRT), cobalt, photon, or proton therapy. When this type of radiation is used, you will likely need to wear a mask that is fitted for you to help you keep still during treatments. This mask can cause anxiety and claustrophobia. Your providers will be able to give you advice to help you with wearing the mask during treatment.
- Internal radiation therapy: A radioactive source is placed inside the body, in or near the tumor. This is called brachytherapy or implant therapy.
Because radiation can affect nearby tissues, there are many potential side effects of radiation for head and neck cancers. Talk with your care team about which type of radiation, if any, you will receive and the potential side effects.
Chemotherapy
Chemotherapy is the use of anti-cancer medications to kill cancer cells. It can be used with radiation therapy (chemoradiation), as the first treatment before chemoradiation, after radiation therapy (called adjuvant chemotherapy), to help with symptoms (called palliative therapy), or to treat cancer that has come back (recurrence).
Chemotherapy medications that may be used are cisplatin, 5-fluorouracil (5-FU), gemcitabine, carboplatin, epirubicin, paclitaxel, docetaxel, capecitabine, and methotrexate. These medications can cause side effects. Ask your medical oncologist which medications would be best for you and at what point during treatment you will receive them.
Targeted Therapy
Hypopharyngeal cancer may be treated with targeted therapies that focus on specific gene mutations or proteins in the tumor. Targeted therapies work by targeting something specific to a cancer cell, which lets the medication kill cancer cells and affecting healthy cells less. Sometimes the “target” is found on a certain type of healthy cell and side effects can happen as a result. An example of a targeted therapy used for this type of cancer is cetuximab.
Immunotherapy
Immunotherapy is the use of a person's own immune system to kill cancer cells. Examples of immunotherapy medications used to treat this type of cancer are pembrolizumab and nivolumab. Your tumor may need to be tested to make sure immunotherapy medications will work for you.
Supportive/Palliative Treatment
Your quality of life is very important during and after treatment for head and neck cancer. Supportive and palliative treatments are used to lessen symptoms or side effects that you may have. Head and neck cancer treatment and the cancer itself can cause:
- Pain: Your care team will help you with medications and other therapies for pain. Radiation, surgery, and a nerve block can help as well.
- Nutrition issues: For some patients, difficulty swallowing, mucositis (sore mouth and throat), loss of taste, or a lack of saliva production may make eating hard or impossible. It is important that you see a dietitian to support you in food and supplement choices, and to keep good nutritional status. If needed, a speech and swallowing specialist can test if you can swallow safely without choking or inhaling food. Many patients will need to be fed through a tube placed in their stomach (called a PEG or ‘G' tube). In most cases, this is only temporary (for a short time).
- Changes in Body Image: Social workers and psychologists may be needed to help you cope with the changes in body image and your role in your family.
- Speech problems: A speech therapist can help you regain as much of your speech as possible, and also give you other ways to communicate.
Clinical Trials
You may be offered a clinical trial as part of your treatment plan. To find out more about current clinical trials, visit the OncoLink Clinical Trials Matching Service.
Making Treatment Decisions
Your care team will make sure you are included in choosing your treatment plan. This can be overwhelming as you may be given a few options to choose from. It feels like an emergency, but you can take a few weeks to meet with different providers and think about your options and what is best for you. This is a personal decision. Friends and family can help you talk through the options and the pros and cons of each, but they cannot make the decision for you. You need to be comfortable with your decision – this will help you move on to the next steps. If you ever have any questions or concerns, be sure to call your team.
You can learn more about head and neck cancer at Oncolink.org.